Dr Stephanie Kaye-Barrett is a physician and consultant rheumatologist based in London. Physiotherapist, Zoe Birch, spoke to her about what rheumatologists diagnose and treat, and the common things they refer for physiotherapy, including osteoarthritis, osteoporosis and hypermobility.
Zoe: What is rheumatology?
Dr Kaye-Barrett: Rheumatology is a specialty concerned with the diagnosis and treatment of people with painful musculoskeletal conditions. There are two general categories – inflammatory and degenerative. Inflammatory would be from the immune system, and would include disorders such as rheumatoid arthritis, systemic lupus erythematosus, and sometimes unclassified inflammatory arthritis. The important thing with these patients is to pick these conditions up early as effective treatments are available.
The second big category is degenerative disease, so “wear-and-tear” arthritis. We get a full and correct diagnosis of this using scans and X-rays, and then usually refer to physiotherapy, hydrotherapy and at the end of the line possibly to orthopaedic surgery.
Zoe: Why would patients see a rheumatologist rather than seeing a surgeon for their problem?
Dr Kaye-Barrett: If there’s a chance you might have inflammatory arthritis then the correct pathway would be to go through a rheumatologist, because an orthopaedic surgeon wouldn’t have the skills to pick up the inflammatory form of arthritis. It’s always safer to go to a rheumatologist first so that the diagnosis can be made. The rheumatologist can make the decision whether it’s inflammatory or degenerative wear and tear. They can then make a subsequent referral to orthopaedics if that’s appropriate. But if an orthopaedic surgeon misses inflammatory arthritis then that’s delaying the patient’s treatment.

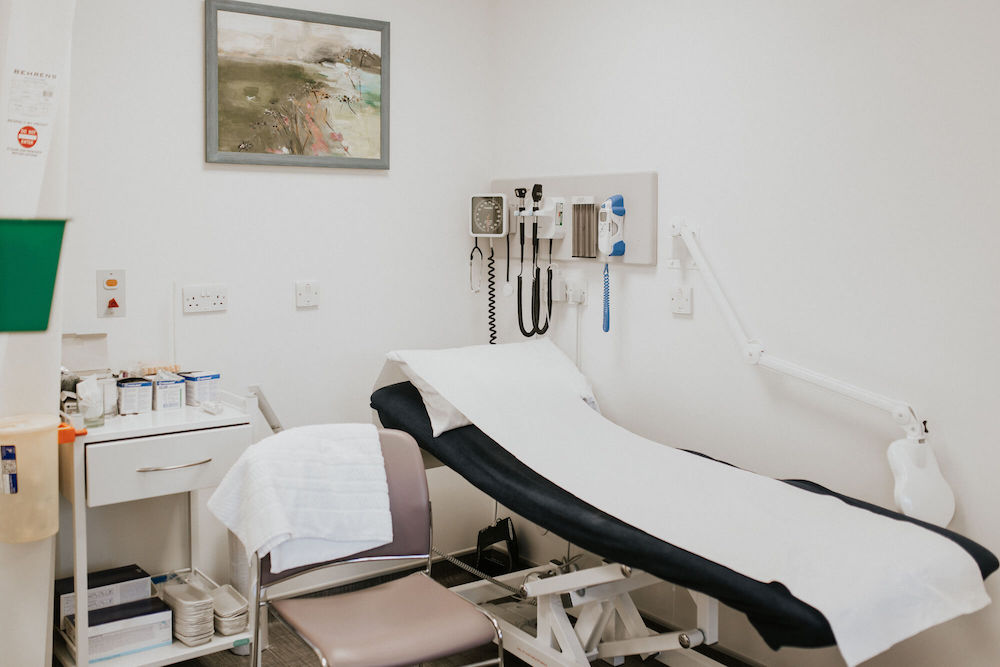
Zoe: And how does physiotherapy complement your work?
Dr Kaye-Barrett: I see a lot of patients with wear-and-tear arthritis and with what’s called soft tissue rheumatism. So, this is another category which is not rheumatoid arthritis. This is very poorly diagnosed and categorised in medicine unfortunately. But the diagnosis is made by an accurate history, then examining the patient, finding a condition such as tendinopathy, plantar fasciitis, or lateral hip pain which is often due to hypermobility or pronation of the feet.
It’s a bit of an art form and you do need to see a rheumatologist to make the diagnosis then refer on to physiotherapy to get the appropriate treatment. This is likely to include muscle release and manual therapy, followed by appropriate exercise to keep the condition under control.
I’d say that about 50 to 60 per cent of my patients are referred to physiotherapy, if not more.
Zoe: What kind of things do you need to hear back from the physio so that you know how the patient’s doing or whether you need to do further investigations down a slightly different avenue?
Dr Kaye-Barrett: Good communication between the physio and the rheumatologist is very important, so that an accurate diagnosis can be passed on to the physio, who then knows where to target treatment. The physio can then also come back with their own ideas about soft tissue, posture, gait and lifestyle problems which are very important.
I’ve had a lot of amazing feedback from physiotherapists. You’re getting a double examination, and they can pick up extra things which may need looking at, or flag up things which should be looked at during a later stage of the treatment. Often a physio will ring and say a patient’s got foot pain now and needs investigation for what’s going on there, for example. So we’ll send the patient back from a scan and then move from there.
Zoe: You mentioned one of the things that you refer to physiotherapy is hypermobility, the other is osteoporosis. Why is it important for people with osteoporosis to have physiotherapy?
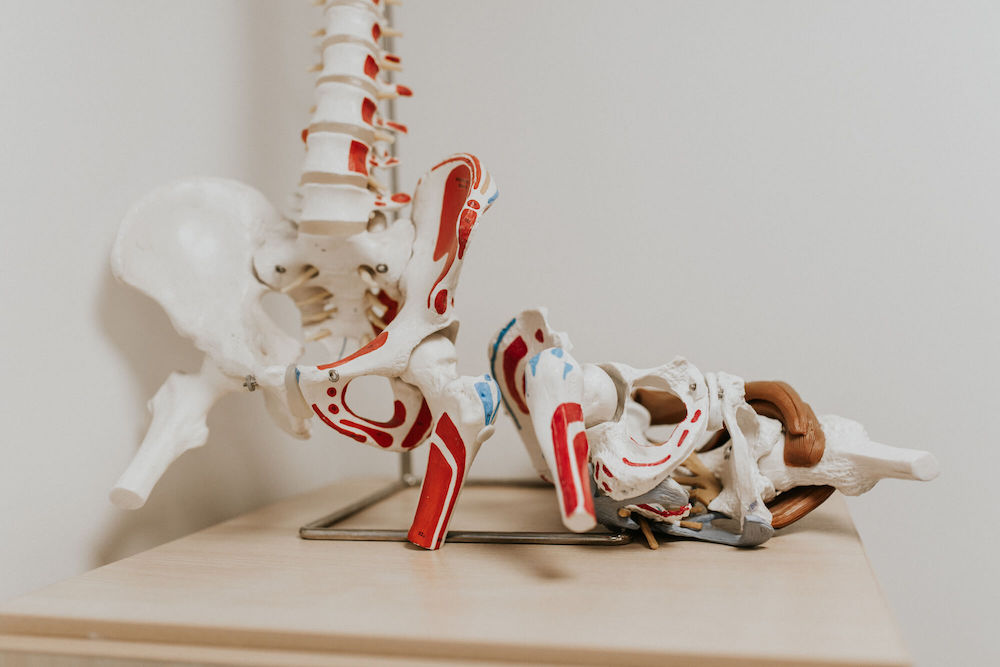
Dr Kaye-Barrett: Osteoporosis refers to thinning of the bones. And people often get it confused with osteoarthritis, which is a wear-and-tear condition. Thinning of the bones can be due to many different factors, one of them being that patients aren’t taking enough weight-bearing exercise. A physiotherapist is in a great position to advise on appropriate exercises to help build the bones. Secondly, the patients may have been sent to the physio for pain management after a fracture resulting from osteoporosis - say a spinal fracture. The physio’s going to work gently with the patient to build up the correct muscles to support the spine and to help gradually rehabilitate them back to normal activities, once they’ve been treated for the osteoporosis medically.

Zoe: A big thing that’s been in the research papers relating to osteoporosis is how important vitamin D is…
Dr Kaye-Barrett: Yes, younger people are becoming very deficient in vitamin D because they’re in offices all the time. They’re not going out into the sun and getting the conversion of inactive vitamin D, which is under the skin, into the active form by sunlight hitting the skin. And then when people go on holiday and have sun exposure they’re wearing really good sun factors, which is great because that prevents cancers of the skin. However, it also prevents the conversion of inactive vitamin D to active vitamin D. So there’s a problem.
I check vitamin D on most people that I see, and the levels which are recommended in the blood are 75 to 200 nano millilitres of vitamin D3 per litre. Many office workers are well below that. A safe thing for most people, if they haven’t got the means to have a vitamin D test, is to take 1,000 international units of vitamin D daily. It’s advisable to have a test just to make sure you don’t get overdoses. That’s very, very unusual in this country though. But I suggest people do get their Vitamin D, calcium and possibly parathyroid hormone levels done, certainly if they’re osteoporotic.
Older people should have screening blood tests for osteopenia – when your bones are weaker than normal – because they’re not going out. They all need vitamin D supplementation, so I’d recommend that they all have a 1,000 international units of Vitamin D3 daily, because if they’re tested, 90 percent of them are vitamin D deficient.
Zoe: And then hypermobility…who typically has that, and how do you manage these patients?
Dr Kaye-Barrett: We see a lot of Middle Eastern and Asian patients who tend to be very hypermobile. Their joints, their connective tissue, their muscles and tendons are very elastic, so they can extend over and above the range of movement of a normal person and do minor injuries to themselves.
Most of the time if they do the wrong type of exercise or sit for prolonged periods their muscles tighten up and get into the wrong position and they get chronic pain in the end. So the message is exercise! I’d suggest pilates because that builds up good core muscle strength. Swimming is great exercise too. A physio is a key part of these people’s treatment and ongoing management to build the right muscles to make sure they’re strong.
If you would like to listen to the full interview click on play button below

If you would like to consult Dr Stephanie Kaye-Barrett, you can contact her at the London Consulting Rooms. She also runs out-patient clinics at the, Lister Hospital, The London Clinic, and 132 Harley Street.
The London Consulting Rooms
2nd Floor
116 Harley Street
London W1G 7JL
020 7730 8508
enquiries@drstephaniebarrett.com